Why Claims Data Underestimates Mental Health Risk
Why Claims Data Underestimates Mental Health Risk
Publication: Employee Benefit News
HealthNEXT President and Chief Medical Officer, Dr. Ray Fabius shares with Employee Benefit News why behavioral health strategies must be grounded in robust data, not assumptions, if employers want to meaningfully improve outcomes and performance. The article underscores that while most employers now offer mental health benefits, too few are tracking utilization, access, and quality metrics closely enough to understand whether those investments are actually working — a gap that can be closed through advanced analytics and integrated population health insights.
Creating a Data-Informed Strategy to Supporting Your Cancer Care Continuum
Creating a Data-Informed Strategy to Supporting Your Cancer Care Continuum
This article, written by Dr. Ray Fabius, is designed for employers, benefit leaders, and their vendor partners who want to use data to improve cancer prevention, detection, treatment, and survivorship across their covered populations. It is adapted from the Greater Philadelphia Business Coalition on Health’s Oncology Resource Guide and summarizes the section authored by Dr. Fabius, “Creating a Data-Informed Strategy to Support Across the Cancer Care Continuum.”
Why cancer care requires a data-informed employer strategy
Employers today have more information than ever to support a healthy, motivated, and productive workforce, including across the cancer care continuum. Applying population health principles helps organizations reduce health risks, ensure rapid access to care, and support employees and family members facing serious illness. When people are thriving, they are less likely to develop cancer, and if they do, they are better able to tolerate treatment and recover.
With the right knowledge and tools, employers can better understand and track key cancer risk factors. Obesity, certain infections such as hepatitis and human papillomavirus (HPV), and chronic conditions like autoimmune disorders and emphysema all play a role. Using data to identify people with these risks and connect them to appropriate screening procedures and care can help reduce complications and improve outcomes over time.
Building on Prevention Science
A strong cancer care strategy is grounded in the four levels of prevention: primordial, primary, secondary, and tertiary. Primordial prevention focuses on improving the work environment and culture, including reducing occupational exposures such as chemicals and radiation. These efforts are within the domain of environmental health and safety experts as well as occupational health physicians and inform decision-making.
Primary prevention aims to eliminate illness by promoting healthy lifestyles, physical activity, smoking cessation, and vaccination rates for viruses such as HPV and hepatitis B. Secondary prevention emphasizes early detection through cancer screening, such as mammography, which can save lives and sometimes avoid more aggressive treatment (lumpectomy). Tertiary prevention ensures access to the best care, including centers of excellence, and provides ongoing support for the growing population of cancer survivors.
Applying the Triple Aim to Cancer Care
The framework of the Triple Aim—improving care, reducing costs, and enhancing experience—offers a clear structure for a cancer continuum dashboard. Employers can track metrics that demonstrate better outcomes, lower per-case costs, and higher satisfaction with cancer care and benefits.
Across the cancer care continuum, distinct phases such as diagnosis, treatment, survivorship, and palliation each deserve tailored metrics. Measuring efforts in awareness, advocacy, navigation, education, coaching, and case management creates a more complete view of how employers, health plans, vendors, point solutions, and EAPs are performing together.
Step 1: Understand Your Cancer Burden
Begin by building a dashboard that illuminates cancer prevalence across your covered lives. Key element examples include:
- Prevalence of cancer-related health risks such as obesity and smoking.
- Acute illnesses associated with cancer, including infections that require strong primary care follow-up.
- Chronic conditions linked to cancer and the extent to which affected individuals access appropriate specialty care.
- Cancer prevalence by diagnostic groupings and across high-cost claimants.
- Cancer prevalence and types among disability and life insurance claims.
This foundation helps employers prioritize where to focus prevention, early detection, and care management efforts.
Step 2: Define Triple Aim Metrics
Next, frame your Cancer Care Continuum Dashboard around effectiveness, efficiency, and experience.
Effectiveness
Example metrics include:
- Reductions in associated health risks
- Improved cancer screening rates
- Higher percentages of early-stage diagnoses
- Increasing cure rates.
- Greater use of EAP services in families coping with cancer and appropriate use of home care and hospice
Efficiency
Example metrics include:
- Reduction in cancer prevalence
- Reduced cost per case
- Decreased cancer-related Hospital days
- Decreased workdays lost
- Decreased disability days due to cancer
- Increased accommodation for cancer patients
- Faster return-to-work timelines
- Fewer lives lost to cancer
Experience
Example metrics, often survey-based, include:
- Greater awareness of the connection of health risks to Cancer
- Greater awareness of the importance of cancer screening
- Greater satisfaction with the cancer care received
Step 3: Activate and Communicate
Capturing data is only the start; leading employers use multiple communication channels to supplement care delivery and educate/activate their workforce. They prioritize cancers that affect large segments of covered lives, for example, focusing programming on breast cancer when data shows it is highly prevalent.
Best practice includes:
- Ongoing review of benefit design and vendor relationships to ensure they collectively support high-quality cancer care
- Convening a vendor summit to align stakeholders on shared metrics can foster collaboration and accelerate improvement
- Guiding timely referrals to complex case management is particularly valuable for employees who lack medical expertise in their families
Step 4: Support Work, Life, and Recovery
A comprehensive cancer care continuum must also address work and life beyond the clinical setting. Employers can track accommodations that allow employees to keep working during treatment or return to work more quickly, recognizing that continued employment may be associated with better outcomes. Monitoring the use of EAP and related support for both patients and family members offers insight into the broader impact of cancer on the household.
These efforts help employees and their families maintain stability and productivity while navigating a cancer diagnosis. Over time, such support improves not only health but also engagement and retention.
Looking Ahead: Evolving the Dashboard
Cancer diagnostics and treatment are advancing rapidly, with new screening tools, surgical techniques, chemotherapies, radiation approaches, and immunotherapies emerging. As these innovations mature, employer cancer dashboards can expand to incorporate new metrics that reflect earlier detection, more targeted treatment, and better long-term outcomes.
Cancer care is increasingly transforming from a purely catastrophic event into a chronic condition managed with maintenance therapy and vigilant follow-up. By continually refining data strategies, employers can increase the likelihood that workers and their families experience cures, sustained health, and a full return to life at work, at home, and at play.
From Health and Wellbeing Insights to Business Outcomes: Turning Employee Health Data into Workforce Strategy
From Health and Wellbeing Insights to Business Outcomes: Turning Employee Health Data into Workforce Strategy
This article explains how employers can use health and wellbeing data to improve workforce performance and business results. Written by the team at HealthNEXT, led by President and Chief Medical Officer Dr. Ray Fabius, it is designed for C suite executives, CHROs, and CFOs who are accountable for workforce strategy and financial performance. It focuses on employer health and wellbeing analytics, including concepts such as the population health continuum, illness burden, and integrated dashboards that link clinical, productivity, and experience outcomes.
Why your organization’s health data isn’t telling a story yet
Most employers are swimming in data from health plans, PBMs, disability carriers, EAPs, and wellness vendors, yet still struggle to answer a basic question: “What does this say about the health of our workforce and our business?” Data feeds often arrive as fragmented cost reports, emphasize lagging indicators, and underplay the sizeable productivity loss associated with poor health — which research suggests is two to three times direct medical spend. As a result, C-suite leaders see line-item costs, not an integrated view of illness burden, risk, and its impact on performance.
A population health continuum view changes this narrative by tracking your people from those who are well to whose at risk, through their bouts of acute illness, to the diagnosis of their chronic disease, and catastrophic illness. When you connect this continuum to business metrics—absenteeism (health-related days lost), presenteeism, disability, safety incidents, and turnover—you can frame health as a performance lever instead of a benefits expense.
Grouping vs. splitting: Framing health prevalence for the C-suite
Most standard reports split data into narrow diagnostic categories that fail to communicate the true magnitude of an enterprise’s challenge. For example, you might see separate prevalence figures for depression, anxiety, attention deficit disorder, substance abuse and alcohol problems; each line looks small on its own and is easy for leadership to dismiss. For most employers grouping the prevalence of these separate conditions demonstrates the remarkable potential influence behavioral health can have on productivity. For many employers this is the number one health related concern for work performance on a population scale.
A grouping approach aggregates related conditions into strategic diagnostic categories that can best direct health and wellbeing efforts to be most impactful. Instead of five separate mental health conditions independently evaluated, you group them and show that one in four employees has a significant behavioral health issue.
- Instead of treating obesity, hypertension, and high cholesterol as isolated findings, you group them as cardiometabolic risk and connect them to cardiovascular claims, disability, and deaths.
- Instead of listing rare catastrophic conditions by name, you group them as “high-cost claimants” and link them back to upstream risk factors and care gaps.
For example, when Dr. Fabius presented a grouped mental health view to one CEO—demonstrating that one out of every four employees had a behavioral health condition—it fundamentally changed the executive’s understanding of the issue and action plan. Grouping shifts the conversation from “we have some depression and anxiety” to “a quarter of our workforce is struggling.”
Waterfall reporting: Following impact from eligibility to outcome
Another reason health and wellbeing investments underperform on paper is that many vendors report only final outcomes or participation rates, not where potential impact is lost along the way. For example, a vendor may report on the percentage of program completions, but only accounting for those who participated, not for the total population who may have benefited from the intervention. Waterfall reporting solves this by mapping the entire journey from the total eligible population to those who actually improve.
A robust waterfall for a diabetes management program, for example, would show:
- Total number of diabetics in your population (e.g., 1,440 people)
- Number with valid contact information who can be invited.
- Number contacted
- Number who enroll
- Number who actively participate
- Number who complete the program
- Number who achieve improved clinical or utilization outcomes after completion

With this line of sight, you can separate employer issues from vendor issues.
- If there is a large drop from total eligible to “invitable,” you likely have data quality or contact information problems that HR and IT must fix.
- If many are eligible and invited but few enroll, you have a marketing and communications problem because employees aren’t appreciating the program’s value.
- If enrollment is strong, but completion and outcomes are weak, the program design and vendor execution needs scrutiny.
Waterfalls turn “the program isn’t working” into “here is exactly where we’re losing people and who owns that step,” which is the level of specificity the C-suite needs to make governance and investment decisions. This approach is no different than how businesses control manufacturing production or supply chain management.
Illness Burden PlacementTM: One page that connects risk to business impact
To truly align health and wellbeing strategy with business strategy, you need a one page view of your organization’s illness burden that integrates multiple data sources. Dr. Fabius refers to this as an Illness Burden Placement™: a single page that orders, by prevalence, the key elements that define the health of your workforce.
That page should show, in grouped form:
- Top risk factors (e.g., obesity, physical inactivity, smoking, high blood pressure)
- Top reasons why the covered lives are accessing care (grouped by major clinical domains, such as musculoskeletal, cardiometabolic, and behavioral health)
- Top reasons why the covered lives are taking medication (such as behavioral health, or cardiovascular)
- Most prevalent chronic conditions
- Most common drivers of high-cost claimants
- Leading causes of disability both short term and long term
- Leading causes of death (derived from life insurance claims)
When you line these up, patterns emerge. For instance, if cardiometabolic risk factors are prevalent, cardiovascular conditions dominate claims and pharmacy, drive disability and high-cost claimants, and are the leading cause of death, you now have a clear, evidence-based rationale to invest in cardiometabolic prevention and care.

From metrics to a corporate health cockpit
The end goal is not a bigger report—it is a cockpit: an integrated collection of key metrics that lets leaders manage workforce health as a strategic asset. A mature cockpit aligns with healthcare quality’s Triple Aim: improving population health, controlling cost and productivity loss, and elevating employee experience and satisfaction.
Effective C-suite ready metrics and visuals share several traits:
- Quantitative with clear numeric values rather than vague ratings
- Actionable, linked to specific levers in benefits, workplace design, and management practices
- Leading where possible (e.g., risk factor prevalence, primary care attachment) rather than purely lagging (e.g., last year’s spend)
- Causally connected, showing how risk leads to disease, claims, productivity loss, and turnover
Visualization matters. Simple, executive friendly tools, such as red/yellow/green streetlights, gauges against targets, and trend arrows help leaders quickly see where they are on track and where intervention is urgent. Site and business unit level scorecards and dashboards can be rolled up into an enterprise level cockpit, creating constructive competition among locations and shining a light on leaders who have built superior cultures of health and safety.

Ultimately, integrated health and wellbeing data should enable you to demonstrate that a healthier workforce is not just “nice to have,” but a persistent source of productivity, resilience, and financial outperformance. When your data is grouped strategically, tracked through waterfalls, and organized into an Illness Burden Placemat™ and health and wellbeing cockpit, the health of your people becomes legible and investable for the C-suite. Effective health informatics converts employee health from “a cost to control” to an investment. Research by HealthNEXT and others have demonstrated that a healthy workforce is a competitive advantage.
Related Resources: NEXTpert Take: Data-driven Population Health Strategies
Building A Culture of Health to Flatten Healthcare Costs
Building A Culture of Health to Flatten Healthcare Costs
Publication: CLEARly Beneficial Podcast
HealthNEXT President and Chief Medical Officer Dr. Ray Fabius joined the CLEARly Beneficial podcast to discuss why building a strong culture of health, safety, and wellbeing is more powerful than price negotiations when it comes to flattening healthcare cost trends. He explains how mid‑market employers can leverage population health expertise, leadership alignment, and HealthNEXT’s evidence‑based assessment and roadmap to turn healthcare into a strategic advantage rather than a strain on the bottom line.
Why GLP-1 Coverage Alone Isn't Enough
Why GLP-1 Coverage Alone Isn't Enough
Publication: Employee Benefit News
HealthNEXT President and CEO Ray Fabius, M.D., shares in Employee Benefit News why simply adding GLP-1 medications to your benefits package is not enough to ensure sustainable results for weight management and health improvement.
Creating an Award-Winning Culture of Health and Wellbeing at DTE Energy
Creating an Award-Winning Culture of Health and Wellbeing at DTE Energy
Authors: Dr. Ray Fabius, MD, and David Kirshenbaum, MBA
A recent article published in Population Health Management highlights how DTE Energy, a Detroit-based energy company with nearly 11,000 employees — 50% of whom are field-based and 49.3% union members—transformed its workplace by fostering an award-winning culture of health and wellbeing. Co-authored by Dr. Ray Fabius and David Kirshenbaum of HealthNEXT, the case study details DTE’s strategic journey to improve employee health outcomes, enhance workplace safety, and strengthen organizational performance. Over a five-year period, DTE achieved a remarkable 75% improvement in their corporate health assessment score, demonstrating significant progress towards becoming a benchmark employer in health and wellbeing.
The Why: A Commitment to People and Purpose
DTE’s vision was rooted in doing “the right thing” for its employees, customers, and community. With a workforce initially burdened by higher-than-average health risks, DTE recognized the need for a comprehensive approach to improve employee health, safety, and engagement.
The company defined wellbeing across four dimensions: physical health, emotional wellness, social connectivity, and financial fitness. By fostering a culture of vitality and care, DTE aimed to empower its workforce and align health initiatives with broader business goals.
The How: A Strategic and Measured Approach
DTE partnered with HealthNEXT to utilize two evidence-based tools—the Employer Health Opportunity Assessment (EHOA) developed by HealthNEXT and Culture Check Site Scans offered through Virgin Pulse. The EHOA provided a top-down comprehensive overview of the organization’s maturity in fostering a culture of health and wellbeing. The Culture Check Site Scan provided a bottom-up view of individual worksites on wellbeing supportive maturity. Together, these tools provided a comprehensive view of organizational strengths and gaps in the existing culture of health and wellbeing.
The initial assessments identified 11 areas of focus to bridge the gaps and achieve best practice over a multiyear strategic plan. These were as follows:
- Embed a best-practice culture of health and wellbeing into DTE’s culture
- Develop and engage an executive committee and champion
- Enhance the workplace environment with a focus on improved nutrition
- Improve population health, including behavioral health
- Market vitality
- Integrate data and analytics
- Train consumers and advocate for them
- Design evidence-based benefits
- Expand on-site services
- Form strategic partnerships and integrate them
- Establish direct provider relationships
Using these focus areas, a comprehensive project plan was developed that included the tasks, milestones, and goals, with a transparent methodology for planning, deploying, improving, and managing over time. Over five years, this roadmap of tactics was refreshed and updated each year, building on successes and ensuring that the correct sequence was followed.
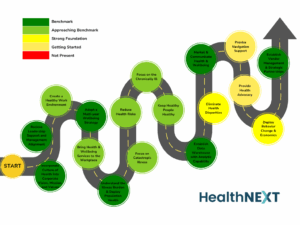
Execution was supported by robust governance structures like the Wellbeing Executive Leadership Committee and a network of 200 local Wellbeing Champions.
The Results: Transformative Impact
DTE achieved significant progress over five years:
- EHOA Score Improvement: The company’s EHOA score rose by 75%, from 386 in 2018 to 675 in 2022—approaching benchmark levels. The EHOA focuses on ten best practice pillars to evaluate a company’s culture of health and wellbeing, producing a score out of 1,000. The benchmark goal is set at 700, indicating a high standard of excellence in health and wellbeing practices. Achieving such a score signifies that DTE is nearing best practice in health and wellbeing, reflecting their significant progress towards becoming a benchmark employer in this area.
- Recognition: DTE received prestigious awards like the C. Everett Koop National Health Award, recognizing their excellence in health and wellbeing initiatives. Since its inception in 1994, only about 70 organizations have received this honor, underscoring its exclusivity and the high standards required for selection.
- Injury Reduction: Musculoskeletal injury rates declined by 36%, while workers’ compensation claims dropped significantly, highlighting improvements in workplace safety.
- Employee Engagement: By 2023, over 89% of eligible employees and their spouses participated in wellbeing programs, including health risk appraisals, biometric screenings and annual checkups.
- Vendor Management and Strategic Partnerships: There was a remarkable 310% increase in the scoring of vendor management and strategic partnerships from 2018 to 2022. This growth underscores DTE’s commitment to leveraging external expertise to enhance its health initiatives.
- Leadership Support and Management Alignment: The score of this particular pillar increased by 109%, reflecting strong leadership commitment.
Notably, employee satisfaction with wellbeing initiatives has surged, with 83% affirming that “DTE cares about my wellbeing.”
Why a Culture of Health and Wellbeing Matters for Employers
- DTE’s case demonstrates that investing in a culture of health and wellbeing delivers measurable benefits:
- Improved employee health which results in reducing healthcare costs.
- Enhanced safety and wellbeing drive performance and retention.
- Recognition as an employer of choice strengthens brand reputation.
DTE’s journey underscores that building a culture of health and wellbeing is not just an ethical imperative but also a strategic advantage. By committing to long-term planning and leveraging proven frameworks like HealthNEXT’s EHOA assessment, organizations can create sustainable change that benefits employees and the bottom line.
Companies that Promote a Culture of Health, Safety, and Wellbeing Outperform in the Marketplace
Companies that Promote a Culture of Health, Safety, and Wellbeing Outperform in the Marketplace
Author: Dr. Ray Fabius, MD
About the Publication
In our recently published peer-review article in the Journal of Occupational and Environmental Medicine, co-authors Raymond Fabius, MD, President of HealthNEXT, and Sharon Phares, Ph.D., found that companies with a culture of health outperform the stock market by an average of 2% per year. Over ten years, their study analyzed the results of a portfolio of publicly traded companies to test the theory that a commitment to employee health, safety, and wellbeing can lead to more robust returns.
How Companies Were Selected
The portfolio companies were identified by the receipt of various health, safety, and wellbeing awards and criteria established from a decade of research at HealthNEXT, the leader in building corporate cultures of health and wellness. The evaluation process included publicly available information such as an established workplace health clinic, a corporate health officer at the senior leadership level, and demonstrated leadership via presentations at health, wellness, and safety conferences.
Results of the Publication
Conclusion
A focus on employee health and wellness resulted in a high return on investment for the portfolio companies and can positively impact business performance.
Companies with healthier workforces have been proven to experience:
- Lower healthcare costs,
- Less absenteeism,
- Higher productivity,
- Less workforce turnover,
- Better talent,
- Less waste, and
- Higher employee engagement levels.
All of these contribute to a competitive advantage in the marketplace and explain the outperformance.
Employers, fund managers, and fund investors would be well served by including strategies that assess a company’s commitment to their workforce’s health, safety, and wellbeing when evaluating investments in their enterprise and portfolios.
8 Ways to Help Support Workplace Health and Wellbeing
8 Ways to Help Support Workplace Health and Wellbeing
Publication: Employee Benefit News
HealthNEXT President, Dr. Ray Fabius shares valuable insights in a new Employee Benefit News article, highlighting the role of leaders in fostering a culture of health and wellbeing.
The Correlation of a Corporate Culture of Health Assessment Score and Health Care Cost Trend
The Correlation of a Corporate Culture of Health Assessment Score and Health Care Cost Trend
Authors: Dr. Ray Fabius, MD., Dixon Thayer, BS., David Kirshenbaum, MBA, and Dr. Jim Reynolds, MD.
Many corporate leaders who promote a culture of health and wellbeing in their organizations face challenges relating their work to tangible economic outcomes. Fortunately, research shows that as the corporate culture of health assessment scores improves, healthcare cost trends moderate.
HealthNEXT executive leaders Dr. Ray Fabius, Dixon Thayer, David Kirshenbaum, and Jim Reynolds, along with Sharon Glave Frazee, Ph.D., MPH, demonstrated a direct linear relationship between a culture of health assessment score (CHAS) and healthcare cost trends. In fact, using the HealthNEXT scoring system on a 1000-point scale; for every 50 points of improvement, there was a 1% reduction in medical trend. This research suggests that there is an immediate and sustainable impact as a company moves from getting started in this pursuit to the point of reaching a best practice score of between 700 and 750.
Read the full study, The Correlation of a Corporate Culture of Health Assessment and Health Care Cost Trend, to learn:
- How corporate health assessments can contribute to lower annual healthcare cost trends
- Examples of corporate health assessment tools
- What is an organizational culture of health
- What specific elements contribute to a healthy corporate culture
Why this study matters
Employers are challenged by what Warren Buffet has called the true corporate tax. For the last few decades, the healthcare costs of their workforce have been trending at an alarming rate of two to three times general inflation, making it difficult to provide salary raises as well as health benefits coverage.
Moreover, according to the Centers for Disease Control, chronic health conditions and unhealthy behaviors reduce worker productivity. Five chronic diseases or risk factors—high blood pressure, diabetes, smoking, physical inactivity, and obesity—cost US employers $36.4 billion a year because of employees missing days of work.
Alternatively, healthy corporate cultures have a workforce with less illness and fewer unhealthy behaviors. As a result, employers with cultures of health and wellbeing spend less on health care without needing to reduce benefit services or shift more costs to their employees.
Purpose of the study
This study aims to determine the relationship between a corporate culture of health assessment score and annual healthcare cost trend by comparing organizations that scored higher versus those scoring lower on the culture of the health continuum.
Methods
HealthNEXT developed, validated, and implemented the Employer Health Opportunity Assessment (EHOA) and the Employer Assessment 50 (EA50) proprietary tools to score a large or mid-sized organization’s culture of health and wellbeing against the benchmark culture of health employers. Benchmark employers have flattened their health cost inflationary trend over many years. Using this score, the team then measured the correlation between CHAS and trends in healthcare expenditures.
EHOA and EA50 are proprietary tools that assess cultural health and wellbeing by analyzing data from a document review, workplace observation, and interviews with senior management, management, and employees to determine elements that contribute to a culture of health.
Study Sample
Data for this study were collected from 21 sets of annual organizational CHAS and healthcare cost trend data points from 12 unique companies.
A total increase year-over-year in total costs was measured for all monies paid to healthcare providers for the organizations’ covered population by both employers and employees. This included medical, prescription drug costs, deductibles, copayments, and coinsurance.
The team identified 21 health score assessments completed between 2011 and 2016 for organizations with available healthcare cost claim data for the same period. Data shows the average score was 459 out of a possible 1000, and the average healthcare cost trend was 5.0%
Analysis
The correlation of CHAS scores with the total healthcare cost trend was strong, and increasing CHAS scores demonstrated lower healthcare cost inflation. In 2015, U.S. healthcare spending for private health insurance increased by 7.2% per person and was projected to increase by 6.8% annually from 2017 to 2025 at the time the article was written. By just modestly improving the culture of health by 50 points out of 1000, the 1% decrease in annual healthcare trends would produce a per-member decrease in healthcare costs of $3999 over a ten-year period.
By implementing best practices, this research implies that it is now possible for employers, large and mid-sized, to control their medical spending and reduce the aggregate health risks and illness burden of their most important asset – their people. Additionally, it is worth noting that other studies referenced in this article calculate that for every dollar saved in direct health care costs, employers save an extra $2.30 in improved performance or productivity.
An Overview of Population Health: Creating Cultures of Wellness
An Overview of Population Health: Creating Cultures of Wellness
Author: Dr. Ray Fabius, MD.
Over the past ten years, population health has gained increased attention, and more organizations are seeking to control healthcare costs while improving health status. Population Health: Creating a Culture of Wellness is a valuable resource for employers, public health professionals, and students looking to understand and lead the charge towards a national culture of health and wellness.
Organizations will benefit from the knowledge shared within the text which outlines the key elements of building a successful culture of health and wellness. Chapter 14 in particular, “Building Cultures of Health and Wellness Within Organizations,” details how to achieve a culture of health and wellness through a vetted seven-step process, including actionable tactics for organizations to adopt.
An Overview of What You’ll Learn
In today’s dynamic healthcare system, Population Health: Creating a Culture of Wellness sheds light on concepts of population health management by exploring strategies for creating a culture of health and wellness and its contribution to true healthcare reform. The reader will gain a thorough understanding of population health from the perspective of practitioners and businesses through various case studies and real-world examples. The textbook is co-authored by HealthNEXT President and Chief Medical Officer Dr. Ray Fabius and is used in medical and graduate programs nationwide.
The reader will gain insights into:
- Implementing organizational culture change
- Population health informatics/analytics
- Health promotion and consumer engagement
- Epidemiology and the impact of social determinants
- Health and wellness vs. healthcare delivery
- The structure and systems of the population health ecosystem
- Value-based payment models
- Policy and advocacy
Dr. Fabius’s Thoughts: Excerpts from Population Health
On the importance of building a culture of health:
“Studying the achievement of companies and organizations who have successfully built a culture of health and wellness can provide great insights for us as a nation. Replicating these best practices on a broader scale can improve the health status of large populations and enhance the quality of life and performance of individuals at work and at home.”
On making the connection between health and wealth:
“Healthier citizens are more productive. The positive outcomes may include more prosperous communities, more involved family members, and more willing civic contributors. As we gradually move toward a national culture of health and wellness, fewer financial resources will be consumed treating illness and more can be directed to keeping well people well.”
Explore the progress towards a national culture of health and how you can help. Order your copy of Population Health today.








